“Your body is a temple, but only if you treat it as one.” — Astrid Alauda
Gynecological health is a cornerstone of overall well-being for women. Understanding your reproductive system is not only empowering but also essential for making informed decisions about your health. In this comprehensive guide, we will explore the intricacies of the female reproductive system, including its key components and how to maintain optimal gynecological health. Knowledge is the first step in ensuring you receive the care and attention you deserve.
The Female Reproductive System: An Overview
“The female reproductive system is a marvel of nature.” — Dr. Jennifer Ashton
Ovaries
The ovaries are essential components of the female reproductive system, serving as both egg-producing organs and endocrine glands. Positioned on either side of the uterus, these small, almond-shaped structures are central to a woman’s reproductive health. Their primary functions include the production and release of eggs during ovulation.
Simultaneously, they are responsible for the secretion of hormones like estrogen and progesterone. These hormones not only govern the menstrual cycle but also influence various aspects of female development and well-being, including secondary sexual characteristics and overall health. From the onset of puberty until menopause, the ovaries play a pivotal role in a woman’s life, regulating her fertility and contributing to the intricate hormonal balance that characterizes the female reproductive system.
Fallopian Tubes
The fallopian tubes are a pair of slender, tube-like structures that connect the ovaries to the uterus in the female reproductive system. These tubes play a crucial role in fertility and conception. When an egg is released from an ovary during ovulation, it is captured by the fimbriae, finger-like projections at the end of each fallopian tube. From there, tiny hair-like structures called cilia help move the egg through the fallopian tube toward the uterus.
If sperm is present in the fallopian tube after sexual intercourse, fertilization of the egg can occur here. Once fertilized, the embryo continues its journey to the uterus, where it can implant and develop into a pregnancy. Fallopian tubes are essential for this early stage of reproduction, and blockages or damage to them can lead to fertility issues. Maintaining the health and function of the fallopian tubes is crucial for a woman’s reproductive well-being.
Uterus (Womb)
The uterus, also known as the womb, is a vital organ in the female reproductive system. It is a pear-shaped, muscular structure located in the pelvis, between the bladder and the rectum. The uterus has several crucial functions. It is where a fertilized egg (embryo) implants and grows during pregnancy, providing a safe and nourishing environment for fetal development. If fertilization does not occur, the lining of the uterus, known as the endometrium, is shed during the menstrual period.
Throughout a woman’s reproductive years, the uterus undergoes monthly cycles of growth and shedding of its lining, known as the menstrual cycle. These cycles are regulated by hormones, primarily estrogen and progesterone. The uterus is an incredible organ that plays a central role in female reproduction and the creation of new life. Understanding its functions and maintaining its health are essential for women’s reproductive well-being.
Cervix
The cervix is a critical part of the female reproductive system, situated at the lower end of the uterus, forming the gateway between the uterus and the vagina. It is cylindrical in shape and has two main functions: providing a passageway for menstrual blood to exit the body and serving as a barrier that keeps the uterus sealed during pregnancy to protect the developing fetus from infections.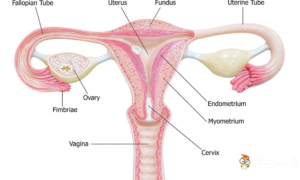
The cervix undergoes various changes throughout a woman’s menstrual cycle and during pregnancy. During ovulation, it produces cervical mucus that facilitates the passage of sperm into the uterus. During childbirth, the cervix undergoes significant dilation and effacement (thinning) to allow the baby to pass from the uterus into the vagina. The health of the cervix is crucial, and regular screenings, such as Pap smears, are essential to detect and prevent cervical cancer. Understanding the cervix’s anatomy and functions is vital for women’s reproductive health and well-being.
Vagina
The vagina, a vital component of the female reproductive system, plays several crucial roles in a woman’s life. It is a muscular, tubular structure extending from the vulva to the cervix of the uterus. One of its primary functions is to serve as a birth canal during childbirth, allowing the passage of the baby from the uterus to the outside world. Furthermore, it enables the expulsion of menstrual blood from the uterus during a woman’s monthly menstrual cycle. Beyond its reproductive functions, the vagina also acts as a conduit for sexual intercourse, facilitating the entry of the penis during sexual activity. Its abundance of nerve endings contributes to sexual pleasure and arousal, making it an integral part of a woman’s sexual experience.
Apart from its reproductive and sexual roles, the vagina also plays a vital role in maintaining overall vaginal health. It produces natural lubrication to ease sexual penetration and prevent discomfort. Additionally, the vagina maintains a slightly acidic environment, which serves as a protective barrier against potential infections and helps maintain a balanced population of microorganisms, including beneficial bacteria. Understanding the vaginal anatomy and its multifaceted functions is essential for women’s reproductive and sexual well-being, underscoring the importance of proper hygiene, regular gynecological check-ups, and a comprehensive understanding of this integral part of the female body.
The Menstrual Cycle: A Natural Rhythm
“The menstrual cycle is a vital sign of overall health.” — Dr. Laura Berman
Menstruation (Period)
Menstruation, commonly known as a period, is a natural and regular process in the female reproductive system. It involves the shedding of the uterine lining, which consists of blood and tissue, through the vagina. This monthly process typically starts during adolescence and continues until menopause. The menstrual cycle, which lasts about 28 days on average, prepares the body for a potential pregnancy. When pregnancy doesn’t occur, hormonal changes trigger the shedding of the uterine lining, leading to menstrual bleeding. Although menstruation is a normal and healthy part of a woman’s life, it can sometimes be accompanied by symptoms like cramps and mood changes. Understanding menstruation health is crucial for reproduction and fertility.
Ovulation
Ovulation is a critical event in the female reproductive cycle, marking the release of a mature egg (ovum) from one of the ovaries. This typically occurs around the middle of the menstrual cycle, roughly 14 days before the start of the next period. Ovulation is triggered by a surge in luteinizing hormone (LH), which causes the ovarian follicle to rupture, releasing the egg.
If the egg encounters sperm during this period and fertilization occurs, it can lead to pregnancy. Ovulation is a vital component of fertility, and tracking ovulation can be helpful for individuals trying to conceive or avoid pregnancy. Various physical and hormonal changes accompany ovulation, including changes in cervical mucus and a slight increase in basal body temperature, making it detectable for those monitoring their reproductive cycles.
Hormonal Fluctuations
Hormonal fluctuations, primarily driven by estrogen and progesterone, play a central role in the menstrual cycle and a woman’s reproductive health. These hormones orchestrate a complex interplay of events, such as the maturation and release of eggs from the ovaries, thickening of the uterine lining, and changes in cervical mucus consistency. These fluctuations not only regulate the menstrual cycle but also impact various aspects of female development and well-being, including secondary sexual characteristics, mood, and overall health.
Understanding these hormonal changes is crucial for managing reproductive health, fertility, and addressing conditions like premenstrual syndrome (PMS) and menopause-related symptoms. For example, estrogen levels rise in the first half of the menstrual cycle, leading to the development of the uterine lining in preparation for a potential pregnancy. If pregnancy doesn’t occur, estrogen levels decrease, triggering menstruation. Progesterone, on the other hand, rises in the second half of the cycle to support the uterine lining and sustain a potential pregnancy. These hormonal shifts not only affect the reproductive system but also influence mood, energy levels, and various bodily functions.
Common Gynecological Conditions
“Awareness is the first step toward effective management.” — Dr. Christiane Northrup
Awareness and understanding of common gynecological conditions are essential for women’s health. Here are some common gynecological conditions:
Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome, commonly known as PCOS, is a hormonal disorder that predominantly affects people with ovaries. It is characterized by various symptoms, including irregular menstrual periods, the presence of cysts on the ovaries, and potential fertility issues. PCOS is associated with hormonal imbalances, particularly higher levels of androgens (male hormones) in the body. While there is no cure for PCOS, lifestyle changes such as dietary adjustments and exercise, along with medications, can help manage its symptoms. These interventions can also be crucial for improving fertility for those trying to conceive.
Endometriosis
Endometriosis is a condition where tissue similar to the lining of the uterus (endometrium) grows outside the uterus. This displaced tissue can be found on the ovaries, fallopian tubes, and other pelvic structures. Endometriosis often leads to severe pelvic pain, especially during menstruation, and can also cause fertility problems. Treatment options for endometriosis include pain relief through medications and, in some cases, surgery to remove the abnormal tissue. Early diagnosis and management are important for improving the quality of life for individuals with endometriosis and addressing potential fertility concerns.
Fibroids
Uterine fibroids are noncancerous growths that develop within the muscular wall of the uterus. They are relatively common and can vary in size. Fibroids can cause a range of symptoms, including heavy menstrual bleeding, pelvic pain or discomfort, and fertility issues, depending on their size and location. Treatment for fibroids is determined by the severity of symptoms and can range from monitoring without intervention to medical treatments or surgical removal of the fibroids. The choice of treatment takes into account the individual’s symptoms and reproductive goals.
Pelvic Inflammatory Disease (PID)
Pelvic Inflammatory Disease, or PID, is an infection that affects the female reproductive organs. It is typically caused by sexually transmitted infections (STIs), such as chlamydia and gonorrhea, but can also occur due to other infections. PID can lead to serious health complications, including chronic pelvic pain, tubal scarring, and fertility problems if left untreated. Timely diagnosis and treatment with antibiotics are crucial to clear the infection and prevent long-term consequences. It’s important for individuals at risk of STIs to practice safe sex and undergo regular screenings to detect and treat infections promptly.
Maintaining Gynecological Health
“Your gynecological health is a lifelong journey.” — Dr. Jennifer Ashton
Maintaining gynecological health is crucial for overall well-being. Here’s a more detailed explanation of each aspect:
Regular Check-ups
Regular gynecological exams, including Pap smears and pelvic exams, are fundamental for women’s health. These exams help detect potential issues early, such as cervical cancer or gynecological conditions like endometriosis or fibroids. The frequency of these exams may vary based on age and individual health history, so it’s essential to discuss with your healthcare provider and follow their recommendations.
Safe Sex
Practicing safe sex is paramount for preventing sexually transmitted infections (STIs) and maintaining reproductive health. Using condoms and other barrier methods can significantly reduce the risk of STIs. If you are sexually active, consider getting regular STI screenings to ensure early detection and treatment if needed.
Contraception
Choosing the right contraception method is a personal decision, and it’s important to discuss your options with your healthcare provider. They can help you find a birth control method that aligns with your reproductive goals and lifestyle. Understanding how to use your chosen method correctly is crucial to its effectiveness.
Healthy Lifestyle
A healthy lifestyle can positively impact gynecological health and overall well-being. A balanced diet rich in essential nutrients supports your body’s functions, including reproductive health. Regular physical activity not only helps maintain a healthy weight but also promotes good circulation and overall vitality. Stress management techniques like meditation, yoga, or deep breathing exercises can reduce stress levels, which may affect menstrual cycles and hormonal balance.
By incorporating these practices into your routine and staying informed about your gynecological health, you can take proactive steps to ensure long-term well-being and early detection of any potential issues. Open communication with your healthcare provider is key to addressing your specific needs and concerns.
Fertility and Reproductive Planning
“Your fertility is a precious asset.” — Dr. Laura Berman
Fertility and reproductive planning are significant aspects of women’s health and family planning. Here’s a breakdown of key considerations in this area:
-
Learn about your fertility and ovulation patterns:
Understanding your menstrual cycle and recognizing signs of ovulation can be valuable if you plan to conceive. Tracking your menstrual cycle, noting changes in cervical mucus, and using ovulation predictor kits can help identify your most fertile days.
-
Charting your menstrual cycle can help if you plan to conceive:
Charting your menstrual cycle through methods like the Basal Body Temperature (BBT) chart and cervical mucus monitoring can provide insights into your fertility patterns, helping you time intercourse for optimal chances of conception.
-
Consider fertility preservation options if you’re facing medical treatments that may impact your fertility:
Some medical treatments, such as chemotherapy or radiation therapy, can affect fertility. In such cases, it’s essential to explore fertility preservation options, which may include egg freezing, embryo freezing, or ovarian tissue preservation. These methods can preserve your ability to have biological children in the future.
-
Explore your options for family planning, including contraception and fertility treatments:
Family planning involves making choices about when and if to have children. It includes considering contraception methods to prevent pregnancy when desired and fertility treatments if conception is challenging. Fertility treatments can include assisted reproductive technologies like in vitro fertilization (IVF) or intrauterine insemination (IUI).
-
Make choices that align with your life goals and values:
Family planning decisions should align with your individual life goals and values. Consider factors such as your career, financial stability, relationship status, and personal desires when making decisions about when to start a family and how many children you want.
Effective communication with healthcare providers, including gynecologists and reproductive specialists, is essential to making informed decisions about fertility and reproductive planning. These professionals can provide guidance, discuss your options, and offer personalized recommendations based on your unique circumstances and goals. Whether you’re focused on understanding your fertility, preserving it for the future, or making choices about family planning, seeking professional guidance can help you navigate this important aspect of women’s health.
Conclusion
“Your body is a temple, but only if you treat it as one.” — Astrid Alauda
Gynecological health is an integral part of a woman’s overall well-being. Understanding your reproductive system, its functions, and common gynecological conditions empowers you to make informed decisions about your health. Remember that regular check-ups, safe sex practices, a healthy lifestyle, and awareness of your fertility can help you maintain optimal gynecological well-being throughout your life’s journey.




